Featured photo: Bobby Jackson, Michigan resident

Written by Tanya Terry
In the United States, African Americans are between four and 17 times more likely to develop sarcoidosis compared with Caucasians. African Americans, in addition to being more frequently affected, are also more severely affected, according to the Oxford Academic American Journal of Epidemiology.
It’s estimated that the prevalence of sarcoidosis in the US ranges between 150,000 and 200,000 with an estimated 1.2 million individuals with sarcoidosis worldwide, according to the Foundation for Sarcoidosis Research.
Some of the individuals who have been diagnosed with sarcoidosis include Mahalia Jackson, Bill Russell, Evander Holyfield and Bernie Mac.
Michigan resident Bobby Jackson was diagnosed with sarcoidosis at age 36. Little did he know that years later he would be experiencing the effects of this disease which is unknown to many, and he couldn’t have imagined how it would intensify the symptoms of COVID-19.
“One summer evening I was sitting at my home computer and began to have cold chills,” Jackson said. “At this point I knew something wasn’t right because it was 83 degrees outside. I immediately told my wife at the time I need to go to the ER. She took me to Providence Hospital, and they took some blood tests and did a chest exam and noticed a nodule on my throat growing very large. It was removed.”
Jackson was put on the schedule for morning surgery. After surgery, Jackson was told he had sarcoidosis, which he, like countless others, had never heard of.

Although there is no cure for sarcoidosis, Jackson was treated with prednisone for years.
A common side effect of prednisone is weight gain. Prednisone can also cause a redistribution of fat to the abdomen, face and back of the neck. The higher the dose and the longer the treatment, the greater these changes tend to be, according to ucsfhealth.org.
“I gained 100 pound despite (the fact) I’m on a weight lost plan once a week; Pulmonologist Physical Therapy.”
Sarcoidosis can affect almost any part of the body. Symptoms vary from individual to individual. So, a variety of different treatment methods is also required. Patients may also experience more than one type of sarcoidosis at the same time.
The most common type of sarcoidosis is pulmonary sarcoidosis, which affects the lungs and affects about 90% of sarcoidosis patients. Cardiac sarcoidosis affects the heart and occurs in a third of sarcoidosis patients.
Jackson was diagnosed with nasal sarcoidosis.
Granulomas-tiny clumps of inflammatory cells-initially developed in his throat, but later started to spread throughout his body.
Jackson said his symptoms got worse after he was diagnosed.
“I start having frequent nosebleeds and discharge while I was at work or at a restaurant. It became unmanageable at times. So I aggressively started seeking out numerous pulmonologists who could help me, and a lot of them just didn’t know what to do.”
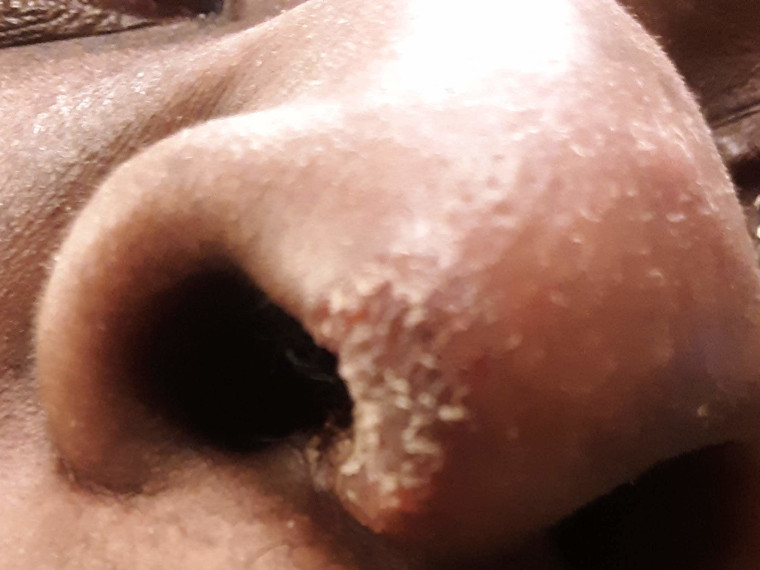
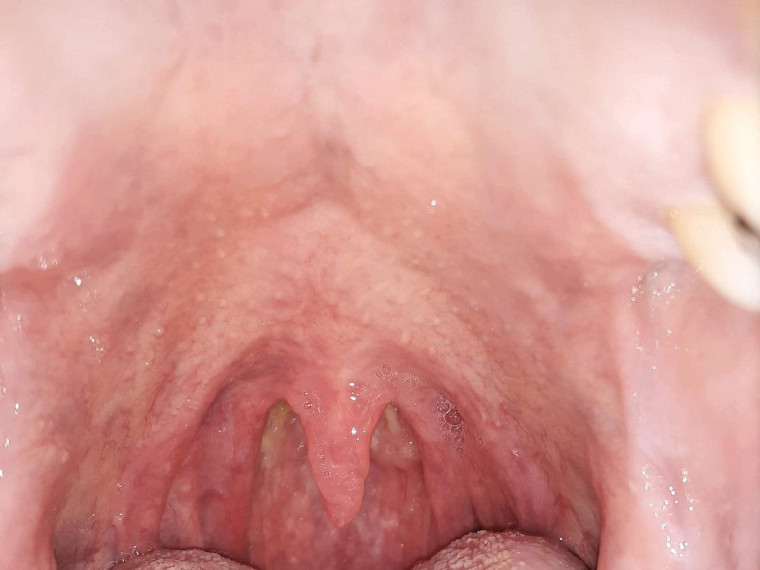
(Sarcoidosis affected Jackson’s nose and also caused inflammation of his throat.)
In Jackson’s case, chronic inflammation lead to fibrosis, which is the permanent scarring of organ tissue.
“Well, initially I did go into remission after two years. But then it came back after going to an eye exam. It showed my eye was inflamed, and I was diagnosed with uveitis.”
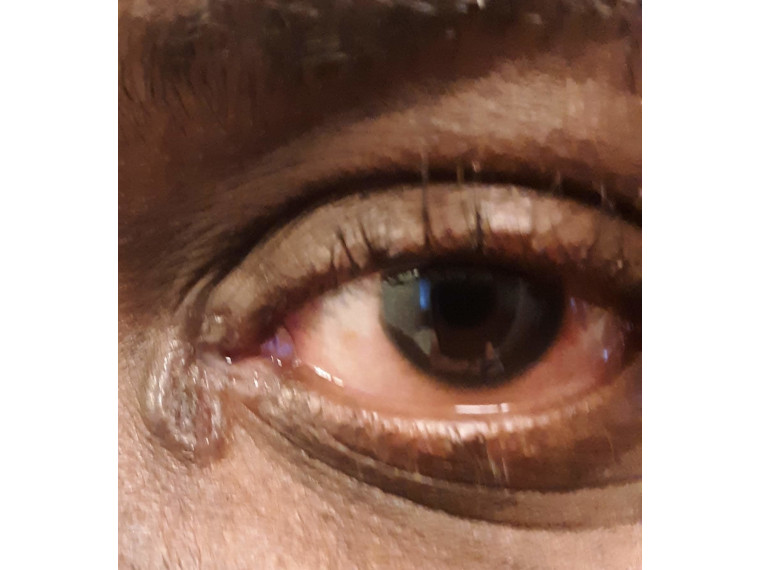
Sarcoidosis came back full force in 2018. That’s when he went to University of Michigan.
Jackson was working as a certified nurse assistant at a hospital. According to Jackson, his work was immensely affected by the disease.
“I was always super exhausted and working a 12-hour shift. It definitely wasn’t the ideal job, but I have a passion for helping people. So, I pushed though it as much as I could until I fell asleep twice at the red light. I was leaving work the next morning at 7 a.m. I had to notify my manager and HR immediately so I didn’t cause an accident and to possibly change hours. They fired me because they said they couldn’t accommodate me.”
Jackson said he “definitely” has advanced sarcoidosis. Advanced sarcoidosis refers to sarcoidosis that is active for two to five years and in which the symptoms worsen despite treatment.
“I’m currently on 20mg (of prednisone) and have to take additional pill, if needed. So, about 40 mg. My nasal cavity often has to be cleaned out at the University of Michigan because it’s constantly inflamed.”
Jackson said when he got COVID-19, it almost took his life.
He was hospitalized from July 21, 2020 until October 21, 2020. COVID-19 damaged his left lung, his right arm and his legs. It caused shortness of breath and heart failure.
More severe cases of sarcoidosis are treated with immune-modulating therapies, making patients more susceptible to infections, including those from COVID-19.
In addition, people with sarcoidosis who have impaired lung function seem to be at greater risk for severe COVID-19 disease, the September 2020 study “Moderate or Severe Impairment in Pulmonary Function is Associated with Mortality in Sarcoidosis Patients Infected with SARS‑CoV‑2” suggests.
Jackson said his life continues to be difficult. He currently must use both an oxygen machine and a walker. His right hand only operates at 30%. He deals with constant numbness in his entire right arm, as well as shooting pain and, at times, sleepless nights.
“I believe if Pfizer can come up with a vaccine 95% effective (for COVID-19) I know they can come up with a cure for sarcoidosis.”
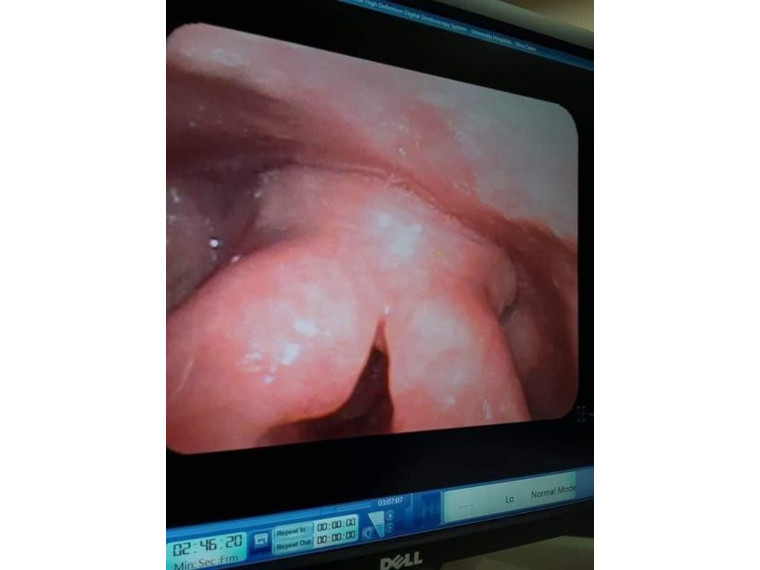
Source: The Foundation for Sarcoidosis Research website
To learn more about sarcoidosis, go to https://www.stopsarcoidosis.org/.

